Is My Tooth Infected?

Your tooth may be infected if you experience severe tooth pain or sensitivity, swelling, or a persistent bad taste in your mouth. An infected tooth can be a serious dental issue that should be addressed promptly to prevent further complications.
Ignoring the signs of an infection can lead to the spread of bacteria, damage to the tooth and surrounding tissue, and potential tooth loss. We will explore common symptoms of a tooth infection, the causes of tooth infections, and the available treatment options.
We will also discuss the importance of seeking professional dental care if you suspect that your tooth may be infected.
Common Symptoms Of Tooth Infection
A tooth infection can cause a range of uncomfortable symptoms that should not be ignored. One of the most common signs of a tooth infection is severe toothache. If you experience a persistent, throbbing pain in your tooth, it could be a sign of infection. Another indicator is sensitivity to temperature. If your tooth becomes especially sensitive to hot or cold foods and drinks, it may be infected. Swollen gums are also a common symptom of a tooth infection. If your gums appear red, swollen, or tender, it could be a sign of infection. Additionally, facial swelling might occur if the infection spreads to the surrounding tissues. Finally, bad breath can be a result of a tooth infection. If you notice an unpleasant odor coming from your mouth, it’s essential to get checked by a dentist to address the infection promptly.
Complications Associated With Tooth Infection
Complications Associated with Tooth Infection
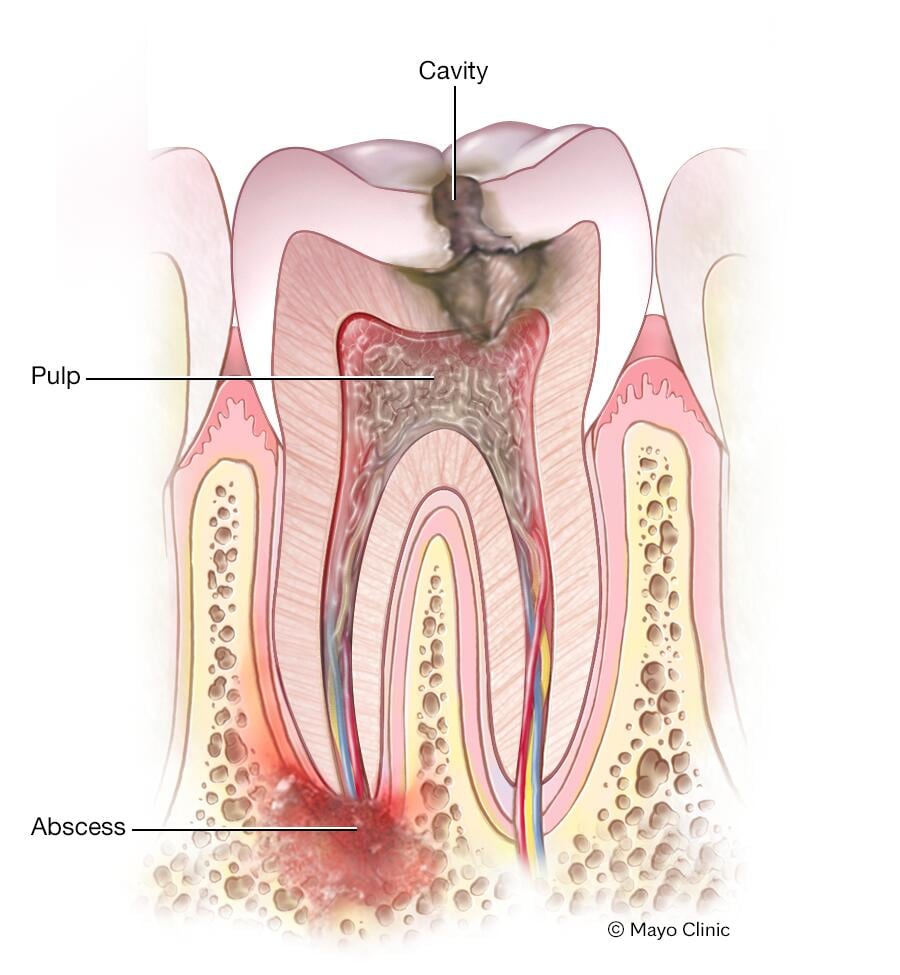
When a tooth becomes infected, it can lead to various complications that require prompt treatment. One major complication is the formation of an abscess, which is a pocket of pus that develops at the root of the infected tooth. Abscesses can cause severe pain and swelling, and if left untreated, they can spread the infection to other teeth.
In some cases, a tooth infection can also lead to a sinus infection. The roots of the upper teeth are close to the sinuses, so an infection in those teeth can spread to the sinuses, causing pain, congestion, and discomfort.
Another complication is the potential damage to the jawbone. The infection can eat away at the bone, leading to bone loss and even the potential for a fractured jaw.
If you’re experiencing symptoms such as severe toothache, swelling, or fever, it’s essential to consult a dentist immediately. Only a dental professional can accurately diagnose and treat a tooth infection, helping to prevent these complications from arising.
Dental Cavities And Decay
Dental Cavities and Decay:
The presence of dental cavities or decay is often an indication of a possible tooth infection. Bacteria play a crucial role in the development of such infections. When oral hygiene is neglected, harmful bacteria accumulate on the teeth, forming a sticky film called plaque. Over time, if not removed through regular brushing and flossing, this plaque can erode the tooth’s enamel, leading to cavities and decay. These openings provide an entryway for bacteria to reach the inner layers of the tooth, potentially causing infections.
Role of Bacteria:
Bacteria present in the mouth feed on sugars and carbohydrates from our diet. They produce acids as byproducts, which gradually dissolve the tooth enamel. Regular consumption of sugary foods and beverages provides ample fuel for these bacteria, increasing the risk of tooth decay and infection. Therefore, it is essential to limit sugar intake and maintain a balanced diet to minimize the growth of harmful bacteria in the mouth.
Failure to Maintain Oral Hygiene:
Poor oral hygiene practices, such as inconsistent brushing and flossing, enable the buildup of plaque and increase the likelihood of tooth infections. Regularly brushing twice a day and flossing helps remove plaque, reducing the risk of enamel erosion and cavity formation. Additionally, scheduling regular dental check-ups allows early detection and treatment of any cavities or infections, preventing them from worsening.
Credit: www.mayoclinic.org
Cracked Or Damaged Teeth
Cracked or damaged teeth can lead to various oral health issues. There are different types of tooth cracks that can occur. One type is damage due to trauma, which can happen from accidents or injuries to the mouth. Another type is caused by chewing hard substances, such as ice or hard candies. Both types of cracks can result in pain and sensitivity, as well as an increased risk of infection. It’s important to address these issues promptly to prevent further damage. If you suspect your tooth is cracked or damaged, it’s essential to consult a dentist for a thorough examination and appropriate treatment. Ignoring the problem can worsen the condition and even lead to tooth loss. Take care of your oral health to keep your smile bright and healthy.
Untreated Gum Disease
Gum disease, if left untreated, can lead to serious consequences. The two main stages of gum disease are gingivitis and periodontitis. Gingivitis is the initial stage and causes inflammation of the gums. If not addressed, it can progress to periodontitis, where the infection spreads below the gum line and can damage the supporting structures of the teeth.
Gum disease has a direct connection to tooth infection. As the infection progresses, it can reach the root of a tooth, leading to an abscess – a pocket of pus that forms at the root of the tooth. This is often a sign that the tooth is infected.
Regular dental check-ups are vital to prevent and detect gum disease early on. Dentists can identify signs of gum disease during routine check-ups and provide necessary treatment. They can also address any underlying dental issues that may contribute to gum disease. Regular cleanings by a dental professional can help remove plaque and tartar, reducing the risk of gum disease and tooth infection.
Root Canal Procedure
In order to determine whether your tooth is infected, it is important to understand the root canal procedure and the steps involved. A root canal is a dental treatment that aims to save a tooth that is severely decayed or infected. During the procedure, the infected pulp inside the tooth is removed, and the interior of the tooth is cleaned and sealed.
The first step in a root canal procedure is to numb the area around the tooth with a local anesthetic. Once the area is numb, the dentist will create a small hole in the tooth to access the pulp chamber. The infected pulp is then carefully removed using specialized tools, and the interior of the tooth is thoroughly cleaned.
After the cleaning process, the dentist will fill the root canals with a biocompatible material called gutta-percha. This material helps to seal the canals and prevent further infection. In some cases, a temporary filling may be placed to protect the tooth until a permanent restoration, such as a dental crown, can be placed.
The success rate of root canal treatment is generally high, with studies showing a success rate of around 85-95%. Recovery time can vary depending on the individual and the extent of the infection. Most people can expect to return to their normal daily activities shortly after the procedure.
If a root canal treatment is not suitable for your specific situation, there are alternative options available. These alternatives may include tooth extraction followed by a dental implant or a dental bridge. It is important to consult with your dentist to discuss the best treatment option for your individual case.
Extraction Of Infected Tooth
When experiencing severe tooth pain, swelling, or discomfort, there is a possibility that your tooth may be infected. In some cases, extraction of the infected tooth may be necessary. There are several reasons why a tooth may need to be extracted, including advanced tooth decay, gum disease, or a dental abscess.
There are two types of extractions: simple and surgical. A simple extraction is performed when the tooth is visible and can be easily removed. Surgical extraction is more complicated and is required when a tooth is impacted, broken, or has extensive damage below the gumline. After a tooth extraction, it is essential to follow proper aftercare instructions to avoid complications and promote healing.
After the extraction, there are various options for tooth replacement, such as dental implants, bridges, or dentures. It is essential to discuss these options with your dentist to decide which is the most suitable for your specific case. Remember, early detection and prompt treatment are key to preventing further dental issues.
Antibiotics And Pain Management
Antibiotics play a crucial role in treating tooth infections. They are prescribed by dentists to eliminate bacteria causing the infection. Amoxicillin, Penicillin, and Clindamycin are commonly prescribed antibiotics for dental infections. These medications help in reducing inflammation, swelling, and pain associated with an infected tooth. However, it is important to note that antibiotics alone may not completely cure the infection, so it is necessary to get appropriate dental treatment alongside.
Managing pain is also an important aspect when dealing with a tooth infection. Over-the-counter pain relievers such as ibuprofen or acetaminophen can help alleviate discomfort until proper dental treatment is obtained. Home remedies like rinsing with warm saltwater, applying a cold compress, or using clove oil can also provide temporary relief. Nevertheless, it is important to seek professional dental care to address the root cause of the infection and prevent any further complications.
Daily Oral Hygiene Practices
Having daily oral hygiene practices is essential to maintain a healthy mouth and prevent tooth infections. Brushing techniques play a vital role in keeping our teeth clean and removing plaque. It is important to use a soft-bristled toothbrush and gentle, circular motions to effectively clean all tooth surfaces. Additionally, don’t forget the importance of flossing. This helps remove plaque and food particles from the spaces between teeth that a toothbrush cannot reach.
Another beneficial practice is mouth rinsing. Using an antiseptic mouthwash helps kill bacteria and reduces the risk of infections. It is recommended to rinse your mouth after brushing and flossing for an extra layer of protection.
By incorporating these daily oral hygiene practices into your routine, you can help prevent tooth infections and maintain a healthy smile.
Regular Dental Check-ups
htmlIn order to maintain good oral health and prevent tooth infections, regular dental check-ups are highly recommended. Getting a thorough examination by a dentist is essential for identifying potential issues at an early stage and taking appropriate action before they worsen. The frequency of dental appointments may vary depending on individual circumstances, but generally, it is advisable to visit the dentist every six months for a routine check-up. These regular visits can detect signs of tooth infections, cavities, gum diseases, and other oral problems. Furthermore, they provide an opportunity for professional dental cleaning, which removes plaque, tartar, and stains that brushing and flossing at home may not effectively address. Professional cleaning not only enhances the appearance of teeth but also minimizes the risk of infection and decay. Overall, keeping up with regular dental check-ups is an important aspect of maintaining good oral health and preventing tooth infections.
Healthy Lifestyle Habits
htmlMaintaining healthy lifestyle habits is crucial for preventing and treating tooth infections. A balanced diet plays a significant role in promoting oral health. Limiting sugar intake is essential as excessive consumption can lead to tooth decay and cavities. Additionally, avoiding tobacco and alcohol is highly recommended, as these substances not only harm overall health but also negatively impact oral health. Smoking and drinking can increase the risk of gum disease and tooth loss. Furthermore, managing stress levels is vital for oral health. Stress can contribute to teeth grinding and jaw clenching, which can cause tooth damage and infections. Practicing stress management techniques such as exercise, meditation, and deep breathing can help alleviate these issues. By incorporating these healthy lifestyle habits, individuals can take proactive steps to prevent and address tooth infections.
| Healthy Lifestyle Habits | Effects on Oral Health |
|---|---|
| Balanced Diet and Sugar Intake | Prevents tooth decay and cavities. |
| Avoiding Tobacco and Alcohol | Reduces the risk of gum disease and tooth loss. |
| Stress Management and Oral Health | Prevents tooth damage and infections caused by teeth grinding and jaw clenching. |
Frequently Asked Questions For Is My Tooth Infected?
How Long Can A Tooth Infection Go Untreated?
A tooth infection can worsen if left untreated, causing severe pain and spreading to other parts of the body. Seeking dental treatment as soon as possible is crucial to prevent complications.
Can You Get Rid Of An Infected Tooth?
Yes, an infected tooth can be removed by a dentist through a procedure called tooth extraction.
How Can I Treat Tooth Infection At Home?
To treat a tooth infection at home, rinse your mouth with warm saltwater, apply a cold compress to reduce swelling, and take over-the-counter pain relievers. Avoid sugary foods, brush and floss regularly, and maintain good oral hygiene. However, it’s important to see a dentist for proper evaluation and treatment.
What Color Is An Infected Tooth?
Infected teeth can appear discolored, usually turning gray, black, or even yellowish.
Conclusion
If you experience persistent pain, swelling, bad taste, or a pulsating sensation in your tooth, it may be infected. Ignoring the symptoms can lead to severe complications. It’s crucial to seek immediate dental care to diagnose and treat the issue effectively.
Don’t hesitate to consult a dental professional who can provide the necessary treatment for your tooth infection. Remember, early intervention is key to preserving your oral health.




